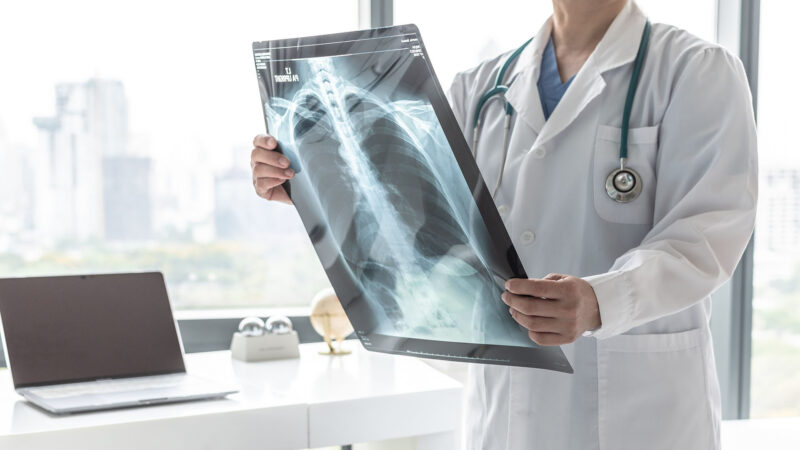
Chronic Obstructive Pulmonary Disease (COPD) represents an umbrella term that includes chronic bronchitis, emphysema, and refractory asthma. It is a progressive disease, meaning it worsens over time, typically leading to increasingly severe symptoms and respiratory complications. It’s crucial to understand COPD, not only because it is the third leading cause of death globally but also because its progressive nature means early detection can significantly affect the prognosis.
Stage 1: Recognizing the Early Signs and Symptoms
Stage 1 COPD, also known as mild COPD, is where the journey usually begins. At this stage, many individuals may be unaware they have the condition as symptoms can be mild or non-existent. The most common symptoms include shortness of breath, particularly during physical activities, a mild but persistent cough, and a tendency to produce more mucus or sputum than usual.
Because these symptoms can easily be mistaken for normal aging or a sedentary lifestyle, Stage 1 COPD often goes undiagnosed. Regular smokers may dismiss these symptoms as a ‘smoker’s cough.’ However, any persistent cough or breathlessness warrants medical attention, as early diagnosis and treatment can slow the progression of the disease.
For individuals diagnosed with Stage 1, the damage to the lungs is minimal, and they have a normal spirometry test, meaning their lung function is at least 80% of the expected value. At this stage, lifestyle changes can significantly impact the course of the disease, making it essential for patients to educate themselves about COPD.
Stage 2: Progression and Impact on Lung Function
As COPD progresses into Stage 2 or moderate COPD, the symptoms become more noticeable. Individuals may experience increased breathlessness during everyday activities like climbing stairs or walking. A worsening cough, increased mucus production, frequent respiratory infections, and fatigue are other common indicators of Stage 2 COPD.
At this stage, the limitations in airflow start to show up in spirometry tests, indicating that lung function has been impaired. Typically, lung function in Stage 2 is between 50-79% of the expected value. While this decline is concerning, it’s crucial to remember that the progression of COPD can be managed effectively with the right care and treatment approach.
Despite the increased symptoms and reduced lung function, some people may still ignore or downplay their symptoms, attributing them to aging or lack of fitness. However, this is the stage where proactive measures and treatment can still significantly slow the progression of the disease, improve quality of life, and extend longevity.
Stage 3: Severe Symptoms and Decreased Quality of Life
Stage 3, or severe COPD, signifies a critical point in the disease’s progression. Symptoms become more severe, with individuals experiencing significant shortness of breath, even during mild activities or at rest. Frequent respiratory infections, chronic cough, and extreme fatigue become common. These escalating symptoms often make everyday tasks challenging, resulting in a decreased quality of life.
The decline in lung function becomes more apparent in Stage 3, with spirometry showing lung function between 30-49% of the expected value. The risks of exacerbations, periods when symptoms become significantly worse, also increase during this stage, sometimes leading to hospitalization.
Even though Stage 3 COPD is severe, it’s essential to note that many treatment options can help manage symptoms, reduce the risk of complications, and improve the overall quality of life. It’s never too late to seek help and make lifestyle adjustments that can make a difference.
Stage 4: End-Stage or Advanced COPD
Stage 4 COPD, also known as very severe or end-stage COPD, is the most advanced stage of the disease. At this stage, symptoms are extreme and can be life-threatening. Shortness of breath becomes so severe that it’s present all the time and makes it very difficult to complete even the simplest tasks. Other symptoms include significant weight loss, lower muscle endurance, and swelling in the ankles, feet, or legs due to a condition called peripheral edema.
In Stage 4, lung function is less than 30% of the expected value, which significantly affects oxygen levels in the blood. This can lead to complications such as respiratory failure and pulmonary hypertension. Exacerbations are more frequent and severe, often requiring hospitalization and sometimes leading to respiratory failure.
However, even in Stage 4, interventions can improve comfort and quality of life. Palliative care focuses on managing symptoms, reducing discomfort, and supporting patients and their families during this challenging time. Early planning for end-of-life care is crucial to ensure patients’ wishes are respected.
Diagnostic Tests and Evaluation
Diagnosis of COPD primarily involves a thorough evaluation of symptoms, risk factors, and a spirometry test. Spirometry measures how much air you can inhale and exhale, as well as how quickly you can exhale, helping to determine lung function and the severity of COPD.
Along with spirometry, doctors may use other tests to diagnose and stage COPD. These can include a chest X-ray or CT scan to visualize the lungs and a blood test called arterial blood gas to measure how well your lungs are bringing oxygen into your blood and removing carbon dioxide.
Although spirometry is the primary tool for staging COPD, the GOLD guidelines also recommend considering symptoms and the patient’s history of exacerbations. This comprehensive approach ensures a more accurate diagnosis and effective treatment plan.
Treatment Options for Stages 1 and 2

While there is no cure for this disease, various treatment options can help manage symptoms, slow disease progression, and improve quality of life. In the early stages of COPD, lifestyle changes are often the first line of treatment. This includes quitting smoking, which is the primary cause of the disease, and avoiding exposure to secondhand smoke and other lung irritants.
Bronchodilators are medications often used to relax the muscles around the airways, helping them to stay open and make breathing easier. Inhaled corticosteroids can also be prescribed to reduce inflammation in the lungs. Pulmonary rehabilitation, a program that combines exercise, education, and support, is highly beneficial in improving fitness and overall well-being.
Early-stage COPD patients may also benefit from a healthy diet rich in antioxidants and regular physical activity, which can strengthen the respiratory muscles and improve endurance. Vaccinations against influenza and pneumonia are also recommended, as people with this disease are more susceptible to these illnesses.
Managing Stage 3
Management strategies in Stage 3 COPD focus on alleviating symptoms, improving quality of life, and preventing complications. Bronchodilators and inhaled corticosteroids continue to be fundamental in managing symptoms. However, additional treatments may be required, such as oxygen therapy for patients with low oxygen levels in their blood.
Pulmonary rehabilitation remains essential at this stage, with customized exercise programs helping to maintain muscle strength and endurance. Patient education about managing symptoms and understanding when to seek medical help is crucial to prevent exacerbations.
Regular check-ups are important in Stage 3 COPD to monitor disease progression and adjust treatments as necessary. Managing associated conditions such as heart disease, anxiety, and depression also play a significant role in the overall treatment plan.
Palliative Care for Stage 4
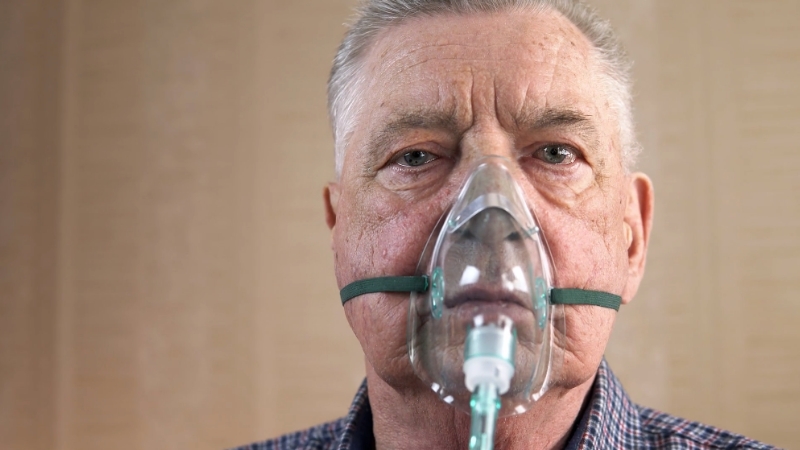
Palliative care plays a pivotal role in managing Stage 4 or end-stage COPD. The goal at this stage is not to cure the disease but to provide comfort, manage symptoms, and maintain the best possible quality of life. This involves a multidisciplinary approach, including doctors, nurses, social workers, and therapists, to address physical, emotional, and spiritual needs.
Treatment at this stage often involves continued use of medications like bronchodilators, inhaled steroids, and oxygen therapy. Non-invasive ventilation may also be used to assist breathing. Adequate nutrition and hydration, pain management, and addressing any other distressing symptoms are central to palliative care.
Emotional and psychological support for both patients and their families is a crucial aspect of care at this stage. Advanced care planning, including discussions about patients’ wishes for end-of-life care, is an important part of palliative care.
Preventive Measures and Lifestyle Changes for COPD Patients
While COPD is a progressive disease, certain preventive measures and lifestyle changes can slow its progression and improve quality of life. Smoking cessation is the most important intervention, as smoking is the primary risk factor for COPD. Other preventive measures include avoiding secondhand smoke and environmental pollutants that can damage the lungs.
Regular physical activity, a balanced diet, and maintaining a healthy weight can significantly help in managing COPD symptoms and improving overall health. Pulmonary rehabilitation and exercises focused on breathing can help strengthen lung capacity and endurance.
Vaccinations are a critical preventive measure for people with COPD. Influenza and pneumonia can cause serious complications for COPD patients, so annual flu shots and pneumococcal vaccines are highly recommended.
The Importance of Early Detection and Regular Monitoring
Detecting COPD in its early stages significantly affects the disease’s progression, making early detection paramount. Anyone with risk factors such as a history of smoking, exposure to secondhand smoke, or exposure to lung irritants should be screened for COPD.
Once diagnosed, regular monitoring of the disease is crucial to adjust treatments as necessary and prevent or manage exacerbations. Regular check-ups allow healthcare professionals to assess how well the current treatment plan is working and make changes if necessary. Spirometry is typically used to monitor lung function over time.
Remember that while COPD is a chronic condition, it is also a manageable one. With early detection, appropriate treatment, and regular monitoring, individuals with COPD can lead fulfilling lives.
Final Words

Understanding the stages of COPD provides valuable insights into this progressive lung disease and highlights the importance of early detection, lifestyle changes, and comprehensive treatment strategies. Though COPD is currently incurable, the right care and management can significantly slow disease progression, improve quality of life, and even extend life expectancy.
Managing this disease is not a one-size-fits-all approach. It’s about individualized care tailored to where each person is in their COPD journey, considering their unique symptoms, overall health, and lifestyle. Collaborating closely with healthcare providers, educating oneself, and being proactive in managing one’s health are keys to living well with COPD.