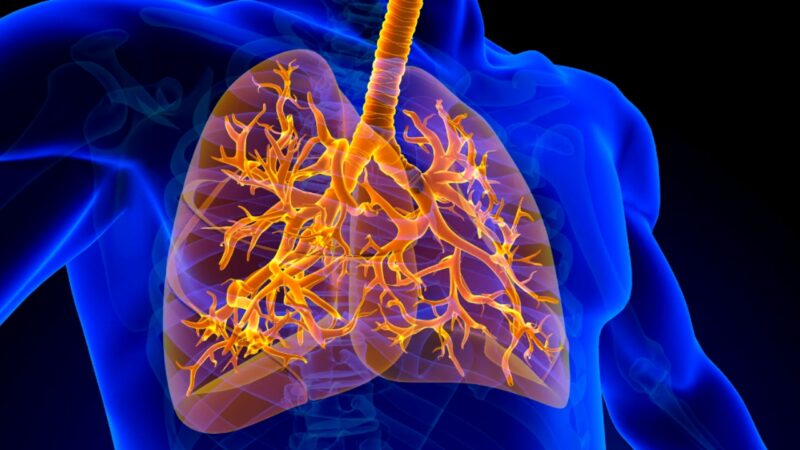
Interstitial Lung Disease (ILD) is a term that encompasses over 200 conditions, all of which cause inflammation and scarring in the lungs. This damage to the lungs’ tissues makes it harder for oxygen to move from the lungs into the body, leading to symptoms like shortness of breath and a dry cough. In this comprehensive guide, we will delve into the causes, symptoms, diagnosis, and treatment of ILD, providing valuable insights to help you understand this complex group of diseases.
What is Interstitial Lung Disease?
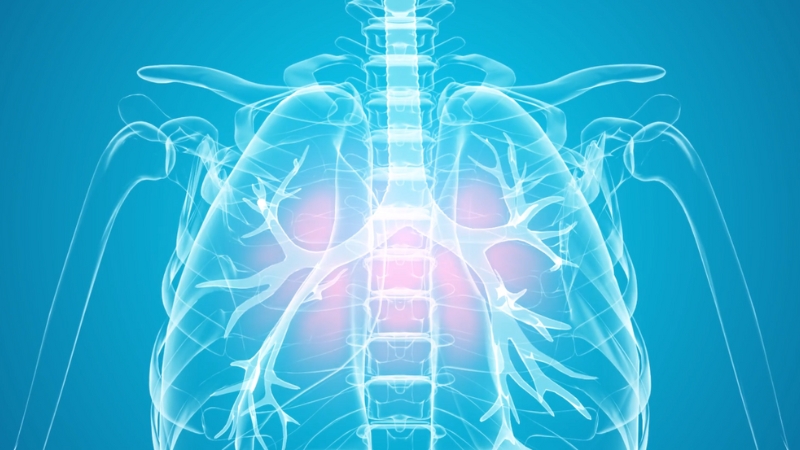
Interstitial Lung Disease (ILD) is a group of conditions that cause inflammation and scarring in your lungs. This damage occurs in the tissues between the small air sacs in your lungs (alveoli) and the blood vessels around them, making it harder for you to move oxygen out of your lungs and into your body. It can be caused by a variety of factors, including medication, radiation therapy, connective tissue diseases, or inhaling harmful substances. Unfortunately, the lung damage caused by Interstitial Lung Disease is often irreversible.
When you have ILD, parts of your lungs that help oxygen get into your blood and out to your tissues are damaged. This scarring in your lungs makes it hard to breathe, and you might have a chronic cough. Lack of oxygen can make you feel tired all the time. If the damage continues to worsen, you can have life-threatening complications, like lung infections and respiratory failure.
There are over 200 types of ILD, with the most common being idiopathic pulmonary fibrosis, followed by diseases caused by occupational exposures or connective tissue disorders. Other examples include asbestosis, silicosis, radiation pneumonitis, and nonspecific interstitial pneumonia.
Interstitial Lung Disease is a condition that affects the lungs, and it’s important to understand the implications of oxygen levels dropping to 87% while sleeping to ensure safety and well-being.
Diagnosing
Diagnosing it involves a physical exam, imaging of your lungs, and testing your lung function. Your healthcare provider will listen to your lungs for any unusual sounds that indicate your lungs aren’t working correctly. They’ll also ask about your medical history, any ongoing conditions, medications you’re taking or have taken in the past, and whether your work or hobbies expose you to certain causes of ILD.
Tests your provider may perform to diagnose ILD include pulmonary function tests, imaging tests like X-rays or high-resolution CT scans, blood tests, bronchoscopy, and biopsy. These tests help determine how well your lungs are working and identify any signs of known causes of ILD.
Treating
While there’s no cure for ILD, treatment usually focuses on treating the underlying disease and improving your symptoms. Your healthcare provider might prescribe physical therapy, supplemental oxygen, or medication to reduce inflammation or slow down the disease. Medications used in ILD treatment include corticosteroids, anti-fibrotic and cytotoxic drugs, biologic drugs, and treatments for gastroesophageal reflux disease (GERD), which can make ILD worse. In severe cases, a lung transplant may be considered.
It’s important to note that some treatments for ILD can weaken your immune system, so your provider will monitor you closely for complications if you’re taking one of these medications.
Living with Interstitial Lung Disease
Living with ILD involves managing your symptoms and preventing further damage. This includes treating any underlying conditions and managing anything that could contribute to ILD, such as GERD. If you work with substances that can damage your lungs or cause an ongoing allergic reaction, you may need to take special precautions.
The outlook for ILD varies depending on the cause and severity. Some people with mild ILD can live normal lives without treatment or with minimal treatment. However, for people with the most severe and rapidly worsening forms of ILD, life expectancy is around 3-5 years after diagnosis. It’s crucial to see your healthcare provider if you’ve had increasing shortness of breath, shortness of breath with exercise, or an ongoing dry cough. The outlook for ILD is best if treated as soon as possible.
Prevention and Risk Factors
While many causes of ILD aren’t preventable, you can reduce your risk by managing underlying conditions and avoiding breathing in harmful substances. This includes wearing a respirator when working around harmful substances like asbestos, metal dust, or chemicals, or around things that can cause chronic allergic reactions. If you have a connective tissue disease or sarcoidosis, talk to your healthcare provider about ways to manage your illness to prevent ILD. Smoking is also a risk factor, so it’s advisable to quit if you do smoke.
The Prognosis

The prognosis of ILD depends on the cause and severity of the disease. Some people with mild ILD can live normal lives without treatment or with minimal treatment. However, for people with severe and rapidly worsening forms of ILD, life expectancy is around 3-5 years after diagnosis. In severe cases, ILD can lead to life-threatening complications, including high blood pressure in your lungs (pulmonary hypertension), collapsed lungs (pneumothorax), lung infections, respiratory failure, and lung cancer.
Conclusion
Interstitial Lung Disease is a complex group of conditions that cause inflammation and scarring in the lungs. While there’s no cure for ILD, understanding the disease, its causes, symptoms, and treatment options can help manage the condition and improve quality of life. It’s essential to have open and honest conversations with your healthcare provider to set your expectations and make a plan to improve your symptoms and have the best quality of life possible.
Remember, each case of ILD is unique, and only your healthcare provider can tell you what to expect in your specific case. Stay informed, stay proactive, and take the necessary steps to manage your health.