When I breathe in, oxygen travels from my lungs into my bloodstream. This level of oxygen in my blood is vital for my body to work correctly.
If my blood oxygen level drops too low, it can lead to significant health problems. Once my cells use up oxygen, they produce carbon dioxide.
My blood then carries this carbon dioxide back to my lungs, and I exhale it through my nose or mouth. My body closely monitors the oxygen saturation in my blood.
If my blood oxygen level, also known as hypoxemia, falls too low, it can cause serious health issues and damage organs like my brain and heart. Low blood oxygen levels could be a sign that my lungs or circulatory system aren’t working as they should
Key Takeaway
- Blood oxygen tests, including arterial blood gas tests and pulse oximetry, are essential for diagnosing and monitoring respiratory conditions and ensuring proper lung and heart function.
- Blood oxygen levels can be measured through a blood draw (arterial blood gas test) for detailed analysis, or non-invasively using a pulse oximeter for immediate oxygen saturation levels.
- Pulse oximeters, available for home use, offer a convenient way to regularly check blood oxygen levels, though they should not replace professional medical evaluation.
- Low blood oxygen levels (hypoxemia) can indicate serious health issues, affecting vital organs like the brain and heart, and require immediate medical attention.
- While low blood oxygen is a possible symptom of COVID-19, it’s not definitive. Testing for COVID-19 is necessary for accurate diagnosis, and a pulse oximeter should not be used as the sole diagnostic tool.
Blood Oxygen Level Test
There are two primary methods for testing blood oxygen levels: a blood draw test and pulse oximetry (using an oximeter). A blood draw test offers more detailed information about oxygen levels compared to an oximeter.
Oxygen Level Blood Draw Test
I measure blood oxygen levels using an arterial blood gas (ABG) test. This test evaluates not just the levels of oxygen and carbon dioxide in the blood, but also the balance of acids and bases, known as the pH balance.
Having incorrect acid levels in the blood can be harmful to health.
Pulse Oximetry
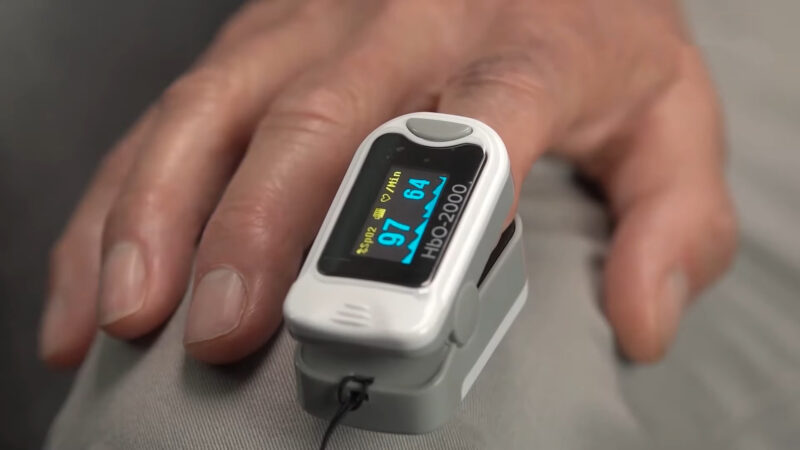
A pulse oximeter measures the oxygen saturation levels in blood using a small clip, typically placed on a finger or toe. This device provides readings of SpO2 levels, indicating the percentage of oxygen-saturated blood, and also shows heart rate.
It’s a fast, non-invasive method for checking if blood oxygen levels are low. Pulse oximeters are widely used in hospitals and are also available for home use.
They can be purchased from pharmacies, and certain stores and websites.
Why do I need to be tested?
You might need a blood oxygen level test for several reasons, as advised by your healthcare provider, particularly in these urgent situations:
- Having difficulty breathing, which is also true for newborns struggling to breathe.
- Suffering from head or neck injuries that could affect my breathing.
- Being infected with COVID-19.
- Developing pneumonia.
- Experiencing carbon monoxide poisoning.
- Sustaining smoke inhalation injuries.
- Encountering repeated episodes of nausea or vomiting.
- Having a drug overdose.
How To Increase It?

To increase my blood oxygen level naturally, I can try these methods:
- Breathing in Fresh Air: I can open my windows or go for a walk outside. This will help increase the oxygen intake of my body and, in turn, raise my blood oxygen level.
- Quitting Smoking: If I stop smoking, my circulation is likely to improve significantly within two to three weeks. Over one to nine months, my breathlessness should decrease, allowing for better oxygen intake.
- Practicing Breathing Exercises: By doing simple breathing exercises like pursed-lip breathing and deep belly breathing, I can open up my airways and boost the oxygen content in my blood.
I can also use a pulse oximeter at home to monitor my blood oxygen level and see if these natural methods are effective. However, I must remember that in severe illnesses like pneumonia or carbon monoxide poisoning, these natural techniques may not be enough to increase my blood oxygen to a safe level.
If I experience symptoms of low blood oxygen (hypoxemia), I should seek immediate medical attention at a hospital.
Blood Oxygen Level Test Details
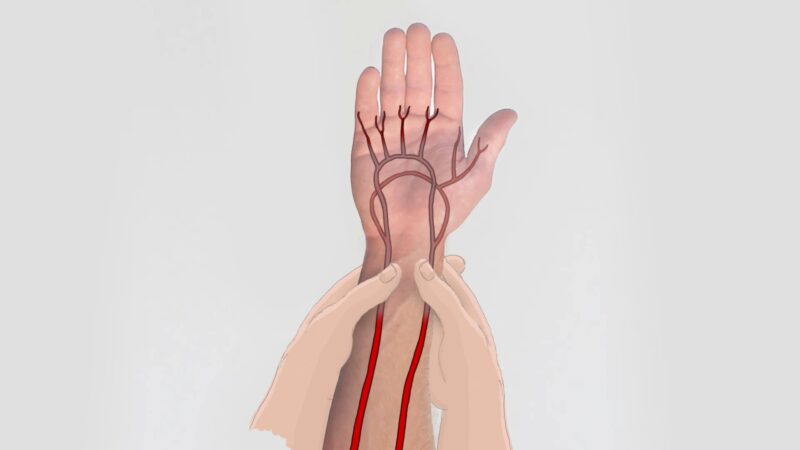
Who Conducts the Test?
A respiratory therapist usually carries out the blood draw for blood oxygen level tests, part of arterial blood gas tests, from an artery in the wrist. They may process the sample themselves or send it quickly to a lab where medical laboratory scientists handle it.
Any healthcare provider can use a pulse oximeter to check blood oxygen saturation level. You can also use a pulse oximeter at home on yourself or others.
Preparation for the Test
Before taking a blood sample from the wrist artery, a respiratory therapist might conduct an Allen test. This involves raising your hand with a clenched fist while the provider applies pressure to wrist arteries for a few seconds, ensuring the arteries are functioning correctly.
If you’re using supplemental oxygen, the provider might turn it off for around 20 minutes before the blood draw, known as a room air test. However, if you can’t breathe without supplemental oxygen, this test won’t be conducted.
Expectations During a Blood Oxygen Level Test

For a blood oxygen level test, part of an arterial blood gas test, the procedure differs from typical blood tests which use a vein. Here, a respiratory therapist will draw blood from an artery, often with higher oxygen levels than venous blood.
The therapist usually samples from the radial artery in the wrist, but sometimes from an elbow or groin artery. In newborns, the sample might be from the heel or umbilical cord.
This process can be more painful than vein blood draws as arteries are deeper and surrounded by nerves. You may feel dizziness, light-headedness, or nausea during the draw.
The steps include:
- You’ll either sit or lie down, and the therapist will locate an artery, possibly using ultrasound.
- They’ll clean and disinfect the area.
- A needle is inserted into the artery for blood collection, which might cause sharp pain.
- Blood is drawn into a syringe.
- After sufficient blood collection, the needle is removed, and pressure is applied to the site to stop bleeding, especially if you’re on blood thinners.
- The site is bandaged, and the procedure is complete.
Test for A Pulse Oximetry Test:
- A pulse oximeter, a small plastic device, is clipped usually to the fingertip.
- It emits infrared light through my skin into the capillary blood.
- The device measures light reflection off hemoglobin to determine blood oxygen levels.
- The oximeter quickly displays the heart rate and oxygen level.
Factors affecting oximeter accuracy include nail polish on the tested digit, bright room lighting, and excessive movement during the test.
Post-Test Expectations
After a blood draw, you might have bruising or soreness at the injection site. It’s advisable to avoid heavy lifting for 24 hours post-test.
Results and Follow-Up
Test reports typically include:
- The test’s name and the specific blood components measured.
- Test result in numerical form.
- The normal range for that test.
- An indication of whether the result is normal, abnormal, high, or low.
Abnormal blood oxygen level test results might indicate:
- Insufficient oxygen intake.
- Inadequate carbon dioxide removal.
- An imbalance in blood pH (too acidic or basic).
A blood oxygen level test alone can’t pinpoint specific conditions. If results are abnormal, the healthcare provider will likely recommend additional tests to confirm or rule out a diagnosis.
When should I know the results of my blood oxygen level test?
The results of a blood sample oxygen level test are usually available right away (within minutes). A pulse oximeter reveals oxygen saturation level within seconds.
When should I call my doctor?
If using an oximeter at home and my oxygen saturation level is at 92% or lower, should call my healthcare provider. If it drops to 88% or lower, I need to get to the nearest emergency room as quickly as possible.
If I have a chronic lung condition like COPD or asthma, I’ll likely need to regularly visit my healthcare provider to ensure my treatment is effective. Should I develop worrying symptoms related to my lung condition, I’ll call my provider right away.
FAQ

Is Low Blood Oxygen a Symptom of COVID-19?
COVID-19 presents with a variety of symptoms, ranging from mild to severe. Not all individuals with COVID-19 will experience low blood oxygen levels. Having a normal blood oxygen level doesn’t necessarily mean you’re free of COVID-19 if other symptoms are present. Conversely, low blood oxygen doesn’t automatically indicate COVID-19.
The definitive way to confirm COVID-19 is through testing. An at-home pulse oximeter, while useful in some scenarios, has its limitations and offers only a partial view of your health status. It should not be used to diagnose COVID-19.
If you’re showing COVID-19 symptoms, consult your healthcare provider promptly.
What Are the Signs of Low Blood Oxygen?
Symptoms of low blood oxygen, or hypoxemia, can vary in severity and differ from person to person. These symptoms include:
- Headaches.
- Shortness of breath.
- Rapid heartbeat.
- Coughing.
- Wheezing.
- Confusion.
- Bluish tint to the skin, fingernails, or lips.
- Cherry red coloration in skin, fingernails, or lips, can indicate carbon monoxide poisoning.
How Does COVID-19 Affect Blood Oxygen Levels?
COVID-19 can impact lung function, potentially leading to decreased oxygen levels in the blood. However, not every case of COVID-19 results in this symptom, and other conditions can also cause low blood oxygen levels.
Can I Monitor My Blood Oxygen Level at Home?
Yes, you can use a pulse oximeter at home to monitor your blood oxygen levels.
Final Words
Understanding and managing blood oxygen levels is crucial for maintaining good health, especially in cases of respiratory illnesses or conditions like COVID-19. Regular monitoring, either through professional medical tests or at-home devices like pulse oximeters, plays a key role in the early detection and management of potential health issues.
Remember, while home monitoring is useful, it should complement, not replace, professional medical advice. Stay informed, stay vigilant, and always consult healthcare professionals for accurate diagnosis and treatment.