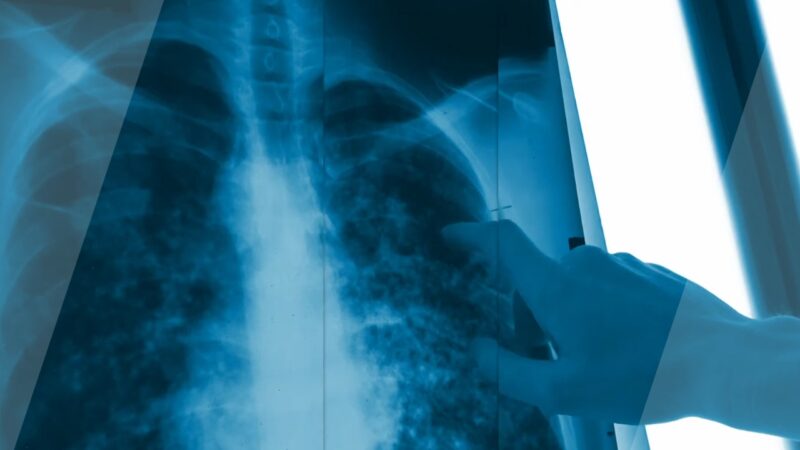
Emphysematous changes refer to the structural alterations in the lungs caused by emphysema, a chronic lung condition characterized by damage to the air sacs (alveoli) in the lungs. One of the diseases that comprise Chronic Obstructive Pulmonary Disease (COPD), a group of lung diseases that cause airflow blockage and breathing-related problems. Understanding emphysematous changes is crucial as it helps in the early detection, diagnosis, and management of the disease, which can significantly improve the quality of life of affected individuals.
Primarily involves the destruction of the alveoli and the loss of lung elasticity. Healthy alveoli are tiny, elastic sacs within the lungs where the exchange of oxygen and carbon dioxide takes place. In emphysema, these air sacs are damaged, leading to fewer and larger sacs that reduce the surface area for gas exchange. This results in shortness of breath and other respiratory symptoms, significantly impacting an individual’s ability to carry out daily activities.
The importance of understanding emphysematous changes cannot be overstated. Early detection and intervention can slow the progression of the disease, reduce symptoms, and improve the quality of life. Moreover, understanding these changes can help in the development of effective treatment strategies and preventive measures, contributing to better management of the disease.
Causes of Emphysematous Changes
The primary cause of emphysematous changes is smoking. Cigarette smoke irritates the airways and damages the alveoli, leading to emphysema. The risk increases with the duration and intensity of smoking. However, not all smokers develop emphysema, suggesting that other factors, such as genetic predisposition, may play a role.
Genetic factors can also contribute to emphysematous changes. A small percentage of people with emphysema have a deficiency in a protein called alpha-1-antitrypsin. This protein protects the elastic structures in the lungs from damage. A deficiency can lead to emphysema, even in people who do not smoke.
Occupational exposure to dust, fumes, and other pollutants can also cause emphysematous changes. Long-term exposure to these substances can irritate and damage the lungs, leading to emphysema. Similarly, exposure to environmental pollutants, such as secondhand smoke and outdoor air pollution, can contribute to the development of the disease.
Pathophysiology
Changes involve the destruction of the alveolar walls, leading to the formation of larger, irregular air spaces. This reduces the surface area available for gas exchange, resulting in decreased oxygen levels in the blood (hypoxemia) and increased carbon dioxide levels (hypercapnia).
The loss of elasticity in lung tissues is another key feature of emphysematous changes. Healthy lungs are elastic and spring back to their original shape after being stretched during inhalation. In emphysema, this elasticity is lost, causing the airways to collapse during exhalation and trapping air in the lungs.
Chronic inflammation also plays a significant role in the pathophysiology of emphysematous changes. In response to irritants such as cigarette smoke, the immune system releases inflammatory cells and enzymes that can damage the lung tissue. Over time, this chronic inflammation can lead to emphysema.
Clinical Features

The primary symptom is shortness of breath, which usually worsens over time and can become severe. Initially, individuals may only experience breathlessness during physical activities, but as the disease progresses, it can occur even at rest. This can significantly limit an individual’s ability to perform daily activities and reduce their quality of life.
A chronic cough is another common symptom. This is often a smoker’s cough, which is usually worse in the morning. The cough is the body’s response to the irritation and damage caused by cigarette smoke or other irritants. It may be dry or may produce sputum, a mixture of saliva and mucus.
Wheezing and chest tightness are other clinical features. Wheezing, a high-pitched whistling sound made while breathing, is caused by the narrowing or obstruction of the airways. Chest tightness, on the other hand, is due to the trapping of air in the lungs, which causes the chest to remain partially expanded, leading to a feeling of tightness or pressure.
Diagnosis
The diagnosis of changes involves a thorough medical history and physical examination, followed by specific tests. The medical history may reveal risk factors such as smoking or occupational exposure to lung irritants. The physical examination may show signs such as wheezing or decreased breath sounds.
Pulmonary function tests are crucial in the diagnosis of emphysematous changes. These tests measure how well the lungs are working. They can detect emphysema even before symptoms appear and can also help determine the severity of the disease.
Imaging tests such as chest X-ray and CT scan can also be used in the diagnosis. These tests can provide images of the lungs, revealing signs of emphysema such as hyperinflation of the lungs or the presence of large, air-filled spaces (bullae).
Complications Associated with It
It can lead to several complications. The most significant is Chronic Obstructive Pulmonary Disease (COPD), a group of lung diseases that includes emphysema and chronic bronchitis. COPD can severely impact an individual’s quality of life and is a leading cause of death worldwide.
Pulmonary hypertension, a type of high blood pressure that affects the arteries in the lungs, is another complication of emphysematous changes. This can lead to right-sided heart failure, also known as cor pulmonale.
Respiratory infections such as pneumonia and influenza are more common and more severe in people with emphysema. These infections can cause further damage to the lungs and can be life-threatening.
Pneumothorax, or a collapsed lung, is another potential complication. This can occur when air gets trapped in the space between the lung and the chest wall, causing the lung to collapse.
Treatment Options

The primary treatment is smoking cessation. Quitting smoking can slow the progression of the disease and improve symptoms. It’s never too late to quit, and there are many resources available to help.
Medications such as bronchodilators and inhaled steroids can also be used to treat emphysematous changes. Bronchodilators help relax and open the airways, making it easier to breathe. Inhaled steroids can reduce inflammation in the lungs.
Oxygen therapy may be needed in some cases. This involves breathing in oxygen through a mask or nasal prongs to increase the amount of oxygen in the blood.
Pulmonary rehabilitation, a program of exercise, education, and counseling, can also help manage symptoms and improve quality of life.
Surgical Interventions

In severe cases of emphysema when other treatments have failed, surgical interventions may be considered. Lung volume reduction surgery involves removing a portion of the damaged lung tissue, allowing the remaining lung to function more efficiently. This can improve breathing and quality of life for certain individuals.
Bullectomy is another surgical option for it. This procedure involves the removal of large air-filled spaces (bullae) that can develop in the lungs in severe emphysema. These bullae can compress healthy lung tissue, impairing its function.
In extreme cases, a lung transplantation may be considered. This involves replacing the diseased lung with a healthy lung from a donor. While this can significantly improve lung function and quality of life, it comes with significant risks and challenges, including the risk of rejection and the need for lifelong immunosuppressive therapy.
Prognosis
The prognosis varies widely and depends on several factors, including the severity of the disease, the individual’s overall health, and whether they continue to smoke. With early detection and appropriate management, individuals with emphysema can lead active and fulfilling lives.
However, emphysema is a progressive disease, and over time, it can significantly impact an individual’s quality of life. It can limit their ability to perform daily activities, lead to disability, and in severe cases, it can be life-threatening.
Mortality rates for emphysema are high, with the disease being a leading cause of death worldwide. However, with advances in treatment and management strategies, survival rates are improving.
Prevention Strategies for Emphysematous Changes
The most effective prevention strategy for emphysematous changes is to never start smoking or to quit if you do. Smoking cessation programs can provide the support and resources needed to quit successfully.
Avoidance of environmental pollutants, such as secondhand smoke and outdoor air pollution, can also help prevent emphysematous changes. This may involve making changes to the home or workplace environment or wearing protective equipment when necessary.
Occupational safety measures can help prevent emphysema in individuals exposed to dust, fumes, and other lung irritants at work. These measures may include the use of protective equipment and regular health monitoring.
For individuals at risk due to genetic factors, genetic counseling can provide information and guidance on managing the risk.
Relationship Between Other Lung Diseases
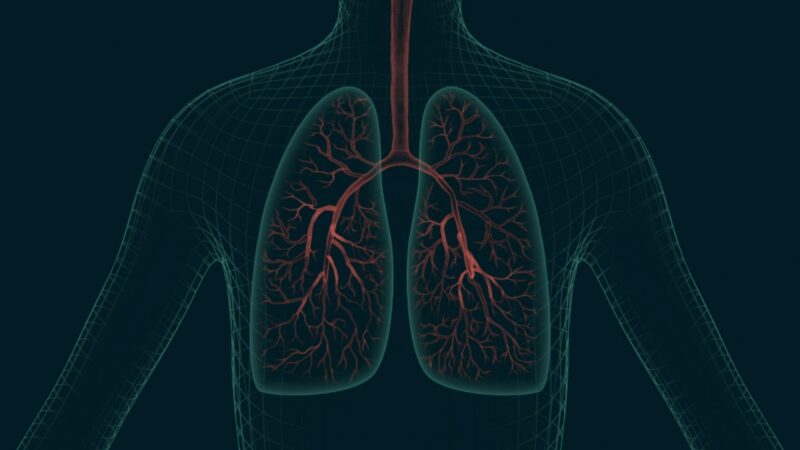
They are often associated with other lung diseases. Chronic bronchitis, a condition characterized by a chronic cough and excessive mucus production, often coexists with emphysema. Both conditions are part of Chronic Obstructive Pulmonary Disease (COPD).
Asthma, a condition characterized by inflammation and narrowing of the airways, can also coexist with emphysema. In some cases, it can be difficult to distinguish between the two conditions, as they share similar symptoms and triggers.
Interstitial lung diseases, a group of conditions that cause inflammation and scarring of the lung tissue, can also be associated with emphysematous changes. These conditions can further impair lung function and exacerbate symptoms.
Lung cancer is another disease that can be associated with emphysematous changes. Smoking, the primary cause of emphysema, is also a major risk factor for lung cancer.
Differences
While emphysematous changes share similarities with other lung conditions, there are key differences in pathological changes, clinical manifestations, and treatment approaches.
In terms of pathological changes, emphysema is characterized by the destruction of the alveoli and loss of lung elasticity, while other conditions may involve different structures in the lungs. For example, in asthma, the primary issue is inflammation and constriction of the airways, not the alveoli.
Clinical manifestations can also differ. While shortness of breath, cough, and wheezing are common in many lung conditions, the nature and timing of these symptoms can vary. For instance, in asthma, symptoms often occur in episodes or “attacks,” while in emphysema, symptoms are typically persistent and progressive.
Treatment approaches also vary. While medications such as bronchodilators and inhaled steroids are used in many lung conditions, the specific types and combinations of medications may differ. Furthermore, surgical interventions such as lung volume reduction surgery or bullectomy are typically reserved for severe emphysema.
Impact on Daily Life

It can significantly impact daily life. Physical limitations, such as shortness of breath and fatigue, can make it difficult to perform everyday activities like walking, climbing stairs, or carrying groceries. Over time, these limitations can lead to disability.
The emotional and psychological effects of living with a chronic disease like emphysema can also be significant. Anxiety and depression are common, often related to concerns about the future, the loss of independence, or the impact of the disease on relationships and social activities.
Social implications can also be profound. Individuals with emphysema may find it difficult to participate in social activities due to physical limitations or the need for oxygen therapy. This can lead to social isolation and a decreased quality of life.
The financial burden of managing emphysema can also be significant. This can include the cost of medications, home oxygen therapy, hospitalizations, and other healthcare services.
Current Research and Advancements in the Field
Current research in the field is focused on developing novel treatment approaches, identifying biomarkers for early diagnosis, and exploring the potential of gene therapy and regenerative medicine.
Novel treatment approaches being explored include new medications, minimally invasive procedures, and personalized treatment strategies based on an individual’s genetic makeup and disease characteristics.
Research is also underway to identify biomarkers, substances in the body that can indicate the presence of disease, for early diagnosis of emphysema. Early diagnosis can lead to earlier intervention and potentially slow disease progression.
Gene therapy, which involves altering the genes within an individual’s cells to treat or prevent disease, is another promising area of research. For example, for individuals with alpha-1-antitrypsin deficiency, a form of emphysema caused by a genetic mutation, gene therapy could potentially provide a cure.
Regenerative medicine, which involves creating or regenerating human cells, tissues, or organs to restore or establish normal function, is also being explored. This could potentially lead to treatments that can repair or replace damaged lung tissue.
Conclusion
Resulting from emphysema, are a significant health concern with a profound impact on individuals and healthcare systems worldwide. Understanding these changes is crucial for early detection, effective management, and the development of new treatment strategies.
The importance of early detection and management cannot be overstated. With timely intervention, the progression of the disease can be slowed, symptoms can be managed, and quality of life can be improved.